Can Exercise Mimic Dopamine Effects on Brain Signals in Parkinson’s Disease?
Parkinson’s disease (PD) is a progressive neurological disorder that affects movement and is partly caused by the loss of dopamine-producing neurons deep in the brain. While medications that replenish dopamine can help control symptoms, researchers are increasingly asking: Can other interventions, like physical exercise, offer similar benefits?
A recent study investigated this by examining how regular, vigorous cycling influences brain activity in people with Parkinson’s. The findings don’t suggest that exercise replaces medication, but they do reveal something intriguing: exercise may partially imitate how dopamine alters the brain’s internal rhythms.
What kind of exercise was used in the study?
The study focused on a specific type called dynamic cycling. It’s not just casual biking; it involves riding a motor-assisted stationary bicycle at a steady, fast pace, usually between 75 and 90 pedal rotations per minute. This style of cycling has been linked to improvements in motor symptoms like stiffness and slowness in people with Parkinson’s. But this study wasn’t about clinical symptoms; it was about electrical signals inside the brain and what they reveal.
 What did the researchers do?
Nine individuals with Parkinson’s, all of whom had deep brain stimulation (DBS) implants, participated in up to 12 cycling sessions over a month. These implants allowed researchers to directly record brain activity from a small structure deep in the brain called the subthalamic nucleus (STN)—a region strongly involved in movement control and a common target in Parkinson’s treatments.
What did the researchers do?
Nine individuals with Parkinson’s, all of whom had deep brain stimulation (DBS) implants, participated in up to 12 cycling sessions over a month. These implants allowed researchers to directly record brain activity from a small structure deep in the brain called the subthalamic nucleus (STN)—a region strongly involved in movement control and a common target in Parkinson’s treatments.
Before and after each exercise session, the researchers measured electrical signals from the brain, called local field potentials (LFPs). They analyzed two types of signals: - Periodic activity: rhythmic brain waves like beta waves. - Aperiodic activity: the background “noise” of brain signals, analyzed through a measure called the 1/f exponent.
What is the relationship between the hindbrain and subthalamic nucleus? Parkinson’s primarily involves the degeneration of dopamine-producing neurons in a midbrain area called the substantia nigra pars compacta (SNc). These neurons produce dopamine, a neurotransmitter vital for controlling movement. They project to other brain regions, notably the striatum. Loss of dopamine in the striatum causes the main motor symptoms of PD: tremors, slowness, stiffness, and balance issues.
The striatum uses dopamine to regulate two pathways: - The direct pathway (which promotes movement) - The indirect pathway (which inhibits movement)
The subthalamic nucleus (STN) is part of the indirect pathway and sends excitatory signals to the globus pallidus internus, which inhibits the thalamus, which in turn controls activity in the motor cortex.
In Parkinson’s loss of dopamine leads to overactivity of the indirect pathway, increasing activity in the STN. This overstimulates the GPi, which then excessively inhibits the thalamus. As a result, the thalamus cannot properly activate the motor cortex, causing slowed and reduced movement.
What did the researchers find? After a month of exercising, consistent changes appeared in brain signals from the dorsolateral part of the STN: - Power of rhythmic activity increased, indicating stronger brain waves. - The 1/f exponent also increased, suggesting the background neural activity became more organized and less noisy.
Interestingly, similar increases in the 1/f exponent occur when people take dopamine-based medication. This suggests that repeated exercise might induce brain states similar to those achieved with drug therapy, at least in certain regions.
However, not all areas of the STN showed changes. The ventral part of the STN remained unaffected, highlighting that the effects were both region-specific and gradual.
What does this mean? This study doesn’t claim that exercise cures Parkinson’s, nor does it prove symptom improvement directly linked to the brain changes observed. Instead, it shows that repeated, structured exercise can produce measurable alterations in brain electrical activity—some resembling the effects of dopamine therapy.
In other words, exercise might help “tune” the brain’s motor circuits to support better movement control, even if the mechanisms differ from medication. By directly measuring brain activity, this study provides early evidence that exercise can influence key brain areas involved in Parkinson’s.
It’s a reminder that improvements in Parkinson’s may come not only from drugs and surgery but also from consistent, targeted physical activity that stimulates the brain in new ways.
There are two ways to counteract the effects of dying neurons, and in both cases, physical activity plays a role. The first involves neighboring neurons forming new synapses to replace those that are lost. The second involves stem cells creating new neurons, but this process is limited by several factors: some neurons have complex structures connecting multiple brain areas, and in older individuals, the supply of stem cells is significantly decreased.

 The authors note that, although their findings are exploratory and cannot be directly applied clinically yet, the identified drugs could be considered for future clinical trials. Indeed, funding should be sought for these future trials, and since it is almost always private investors who finance clinical trials, they would require more information before making any commitments.
The authors note that, although their findings are exploratory and cannot be directly applied clinically yet, the identified drugs could be considered for future clinical trials. Indeed, funding should be sought for these future trials, and since it is almost always private investors who finance clinical trials, they would require more information before making any commitments.
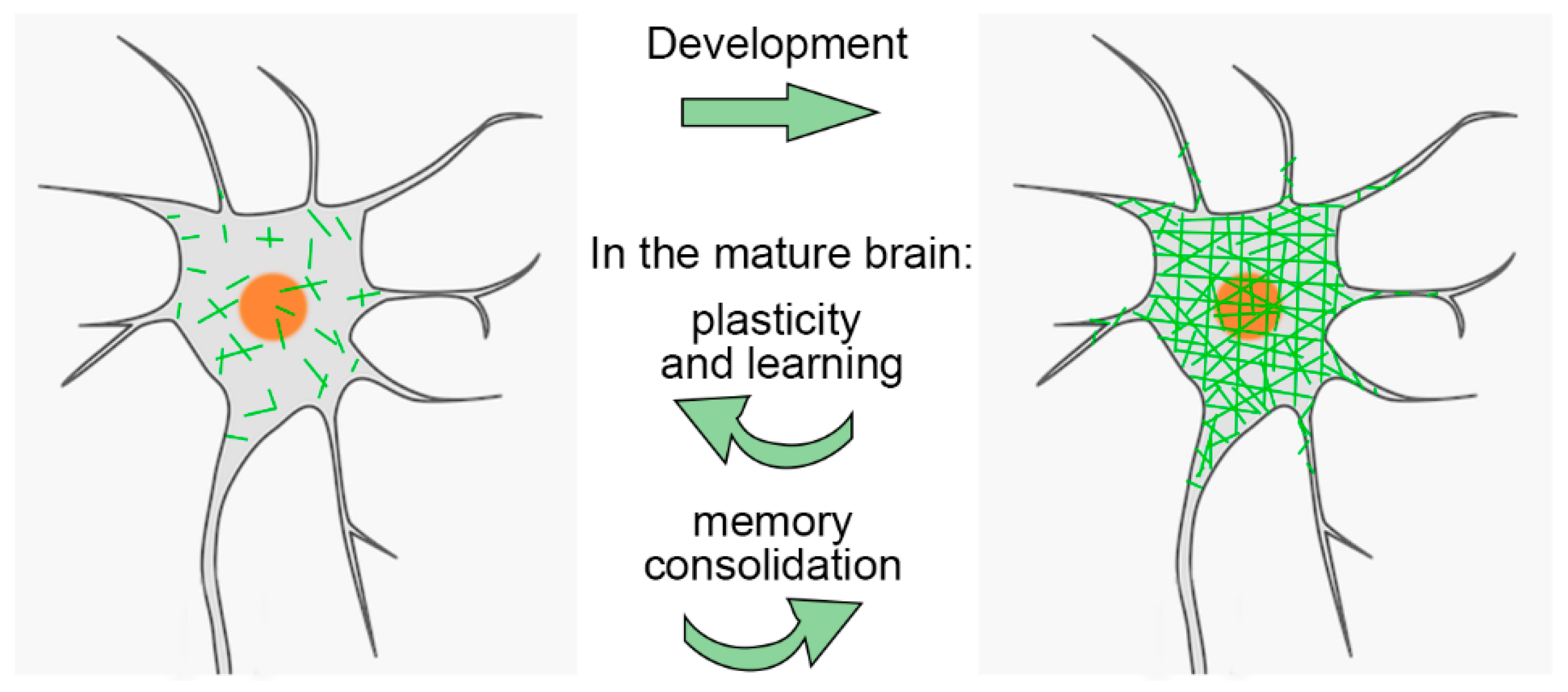 PNNs are especially important during brain development. They help close the "critical period" of heightened plasticity in childhood. Interestingly, while PNNs are degraded in adults, this plasticity can be partially restored. For example, PNN removal can promote recovery in stroke models
PNNs are especially important during brain development. They help close the "critical period" of heightened plasticity in childhood. Interestingly, while PNNs are degraded in adults, this plasticity can be partially restored. For example, PNN removal can promote recovery in stroke models This study investigates whether acupuncture has any impact on long-term health outcomes, such as mortality, disease progression, or complications, in individuals newly diagnosed with Parkinson’s disease (PD) in South Korea. Indeed, it is unclear what constitutes an effective acupuncture session for Parkinson's disease, and individuals interested should receive at least one session every two months. It is commonly believed that in PD, reduced mobility due to tremors, postural imbalance, and rigidity likely contributes to poor circulation and decreased gastrointestinal motility, leading to bowel obstructions and impaired swallowing, which can, in turn, result in recurrent aspiration pneumonia. The benefits may arise from the fact that people with PD might find it easier to move.
This study investigates whether acupuncture has any impact on long-term health outcomes, such as mortality, disease progression, or complications, in individuals newly diagnosed with Parkinson’s disease (PD) in South Korea. Indeed, it is unclear what constitutes an effective acupuncture session for Parkinson's disease, and individuals interested should receive at least one session every two months. It is commonly believed that in PD, reduced mobility due to tremors, postural imbalance, and rigidity likely contributes to poor circulation and decreased gastrointestinal motility, leading to bowel obstructions and impaired swallowing, which can, in turn, result in recurrent aspiration pneumonia. The benefits may arise from the fact that people with PD might find it easier to move. The authors focused on adiponectin, an adipocytokine, i.e. a molecule produced by adipose tissue, which is involved, among other things, in the regulation of lipid and glucose metabolism. Adiponectin modulates inflammatory cascades by modifying the action and production of inflammatory cytokines, but the link between adiponectin and Parkinson's disease is not obvious unless we consider that Parkinson's disease is due to a metabolic disorder. The relationship with the soluble tumor necrosis factor receptor (sTNFR) is even less obvious. Nothing in the article explains why these two molecules were studied.
The authors focused on adiponectin, an adipocytokine, i.e. a molecule produced by adipose tissue, which is involved, among other things, in the regulation of lipid and glucose metabolism. Adiponectin modulates inflammatory cascades by modifying the action and production of inflammatory cytokines, but the link between adiponectin and Parkinson's disease is not obvious unless we consider that Parkinson's disease is due to a metabolic disorder. The relationship with the soluble tumor necrosis factor receptor (sTNFR) is even less obvious. Nothing in the article explains why these two molecules were studied.