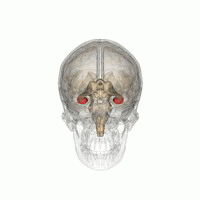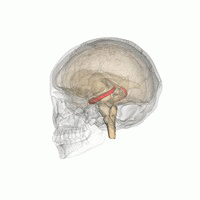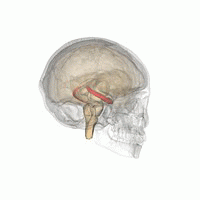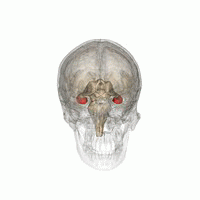
Two patients with familial amyotrophic lateral sclerosis (ALS) and mutations in the gene encoding superoxide dismutase 1 (SOD1) were treated with a single intra-thecal infusion of adeno-associated virus encoding a microRNA targeting SOD1. Unfortunately it did not went well for the patients, but there are many interesting observations in this article. One of them is that one of the patient had an infection of Borrelia burgdorferi, a tick-borne spirochete bacterium also responsible for causing Lyme disease, which was discovered during the course of the disease.
Patient 1 had transient improvement in the strength of his right leg, a measure that had been relatively stable throughout his disease course, but there was no change in his vital capacity.
Patient 2 had stable scores on a composite measure of ALS function and a stable vital capacity during a 12-month period.
Patient 1
During the month of February 2017, Patient 1, a 22-year-old man, began to notice weakness in his left leg. He had the same SOD1 missense mutation (SOD1-A5V) as his mother, who had died from ALS at the age of 45 years. In March 2017, his slow vital capacity was 100% of the predicted value, and his ALSFRS-R score was 42. The flexion strength in his left hip was MRC grade 3, which indicated that he could move the limb against gravity. He could not bear full weight on his left heel or toes though.
On July 19, 2017, he received a single intrathecal infusion of 4.2×1014 vector genomes of AAV-miR-SOD1 along with an intravenous bolus of methylprednisolone (1.0 g); the latter was repeated the following day. Oral prednisone (at a dose of 60 mg per day) was then initiated, with planned tapering during a 4-week period. At that time, there was no plantar flexion or dorsiflexion in the left ankle ; the left knee flexion and extension could move only with gravity eliminated; The strength of the right leg and both arms was normal, as were sensory function and cognition.
Three weeks after the infusion, he had transient tingling in both hands, and 1 week later, he reported having a feeling of painful “electric shocks” in his left foot. The prednisone dose, which had been tapered to 10 mg per day, was increased to 30 mg.
Twenty-four weeks after treatment (46 weeks after the onset of ALS symptoms), the patient’s ALSFRS-R score was reduced to 38 from the baseline level of 42. The loss of strength in the left leg continued.
But at 12 months after treatment (nearly 18 months after the onset of ALS symptoms), the patient had transient improvement in the strength of his right leg, and could propel himself in a wheelchair using the right leg. However vital capacity was further reduced to 21% of the predicted value. At 14 months, he regained the ability to extend and flex the fingers of the left hand, a function that had been absent for the previous 20 weeks.
Lymphocytic meningoradiculitis, also known as Bannwarth syndrome, is a neurological disease characterized as intense nerve pain radiating from the spine. The disease is caused by an infection of Borrelia burgdorferi, a spirochete bacterium.
The patient died of respiratory arrest 15.6 months after the initiation of treatment and 20.5 months after the onset of ALS symptoms. The AAV-miR-SOD1 viral genome was detected in the cervical and lumbosacral spinal cord parenchyma. As compared with a baseline SOD1 level of 120 ng per milliliter in the CSF, the level was 102 ng per milliliter at 8 weeks and 120 ng per milliliter at 41 weeks
There were a loss of motor neurons in the cervical, thoracic, and left lumbosacral spinal cord but relative sparing of motor neurons in the right lumbosacral spinal cord.
The cortical ribbon in the primary motor–sensory cortex was moderately gliotic. Glial scar formation is a reactive cellular process involving astrogliosis that occurs after injury to the central nervous system.
Pyramidal neurons had pyknotic nuclei and hypereosinophilic cytoplasm, findings that were consistent with acute hypoxic–ischemic injury. Hypoxia is a condition in which the body or a region of the body is deprived of adequate oxygen supply at the tissue level. Pyknosis, is the irreversible condensation of chromatin in the nucleus of a cell undergoing necrosis or apoptosis.
The authors hypothesized that intrathecal infusion of this viral vector can trigger an adverse inflammatory response, as has been reported in some studies after the intravenous administration of AAV9 in animals.
The scientists cannot conclude that suppression of SOD1 played a role in his clinical course, since such improvements in function may have reflected recovery from meningoradiculitis.
Patient 2
For patient 2, during the year before therapy, his functional status had been stable, with ALSFRS-R scores averaging close to 28. For a year before treatment, his slow vital capacity had ranged from 42 to 58% of the predicted value;
As meningora-diculitis developed after treatment in Patient 1 and they suspected some relation between the two events, the scientists aimed to suppress B-cell activity and T-cell function with rituximab (at a dose of 375 mg per square meter of body-surface area), which was initiated in late August 2018 in weekly intravenous infusions for 3 weeks and with intrave-nous methylprednisolone (at a dose of 125 mg before each dose of rituximab and 1 g on the day of AAV-miR-SOD1 infusion).
Beginning at the initiation of study treatment, the patient began receiving daily oral sirolimus (6 mg). The day after treatment, oral prednisone (0.5 mg per kilogram of body weight) was initiated; sirolimus and prednisone were continued for 6 months.
On September 17, 2018, the patient received an intrathecal infusion of 4.2×1014 vector genomes of AAV-miR-SOD1.
On the day after treatment and at weeks 12 and 17, he received intra-venous immune globulin (at a dose of 0.4 mg per kilogram) in response to a decrease in the serum IgG to a level of less than 700 mg per deciliter, which had been induced by rituximab.
60 weeks after treatment, the ALSFRS-R score was 24, signifying worse overall function.
At 65 weeks after therapy, the slow vital capacity score value was 62% .
In contrast to the clinical course of Patient 1, the immuno-suppressive regimen in Patient 2 blunted the generation of neutralizing antibodies, antiviral antibodies, and T-cell response to the viral capsid. As of May 18, 2020, his disease course was stable, with a functional measure of 24 at 90 weeks after treatment. A course that could be typical of the slow disease progression in patients with his SOD1 genotype, so no clinical conclusions can be made about the treatment effects.
Conclusion
It is very important for the scientific knowledge acquisition process to publish failures. This study is in this respect important, but it is a quite rare publication that describes also other aspects of the story. If intrathecal genetic therapies incur an increased risk of a Borrelia burgdorferi based disease, this is an extremely important fact.