An adequate blood supply is essential for normal brain function. On the other hand, deficits in cerebral blood flow and dysfunction of the blood-brain barrier are early signs of neurodegenerative disorders in humans and animal models.

A sufficient supply of blood from the 86 billion neurons in the human brain is obtained through a large, well-regulated vascular network of arteries, arterioles, capillaries, venules and veins up to approximately 600 km (400 miles) in length. Neural activity triggers an increase in the regional supply of oxygenated blood within milliseconds. This is called either haemodynamic response or reurovascular coupling.
Two new studies describe the elements of neurovascular physiology that make this feat possible. One, published in Nature on February 19, 2020 and edited by Chenghua Gu at Harvard Medical School, reports that the endothelial cells lining the arterioles have a myriad of entries, called caveolae, which somehow control the rapid dilatation of the arterioles in response to neural stimulation. The other, published on January 20 in Nature Communications and directed by Martin Lauritzen of the University of Copenhagen, describes specialized sphincters that control blood flow from arterioles from the brain into its large capillary beds.
In addition to Alzheimer's disease, the cerebrovascular system has been implicated in the pathogenesis of frontotemporal dementia, Parkinson's disease, Huntington's disease, amyotrophic lateral sclerosis (ALS), multiple sclerosis and others neurodegenerative conditions such as HIV-induced neurocognitive disorder.
ALS patients also develop perfusion deficits in the fronto-parietal cortex.
The conventional model postulates that neurovascular coupling is mediated by vasodilator factors derived from neurons that directly relax the arterial smooth muscle cells. However, according to recent work, it seems that brain endothelial cells can also detect neuronal activity. Perhaps then the vasodilator signals first act on the brain endothelial cells before being relayed to the arterial smooth muscle cells.
Chow et al. explore this potential neurovascular coupling mediated by brain endothelial cells by adopting a very elegant approach. They focused on the somatosensory cortex of laboratory mice, where stimulation of the whiskers reliably triggers neural activity, dilated vessels and blood flow. They show that conventional detection of nitric oxide in smooth muscle cells is insufficient for complete neurovascular coupling.
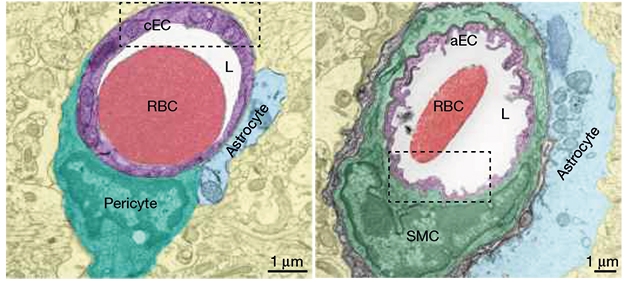
Instead, the caveolae enriched with arteriolar cerebral endothelial cells are also necessary for efficient coupling. Using various cell-type specific mouse models and the overall knockout and overexpression gene, they confirm that the celloles in cerebral endothelial cells - not arterial smooth muscle cells - are necessary for neurovascular coupling.
These discoveries inspire fascinating questions to understand the biology of the cerebrovascular system in terms of health, aging and disease.

