Many ALS patients have noticed that their patients seem to share a particular skin type. Studies have shown that ALS patients often exhibit small fiber neuropathy in the skin, contributing to symptoms such as impaired thermoregulation, abnormal sweating, and sensory disturbances (e.g., numbness, and pain). Similar skin changes have been observed in diseases such as Parkinson's disease and Alzheimer's disease, suggesting that skin biomarkers could contribute to the early diagnosis and monitoring of ALS.
The article reviewed here is a review of this phenomenon, which rarely receives scientific attention. While the focus of the article is on early diagnosis of ALS, scientists, and physicians are not necessarily pleased that ALS is a disease far more complex than motor neuron disease, as this makes it difficult to conceptualize and makes the design of therapeutic strategies more challenging.
One factor that may explain this is that the skin and the nervous system share a common embryonic origin. The skin is composed of the epidermis, dermis, subcutaneous tissue, and appendages (such as sweat and sebaceous glands). In patients with ALS, the skin exhibits a soft, leathery texture, as well as a phenomenon called delayed return (DRP).
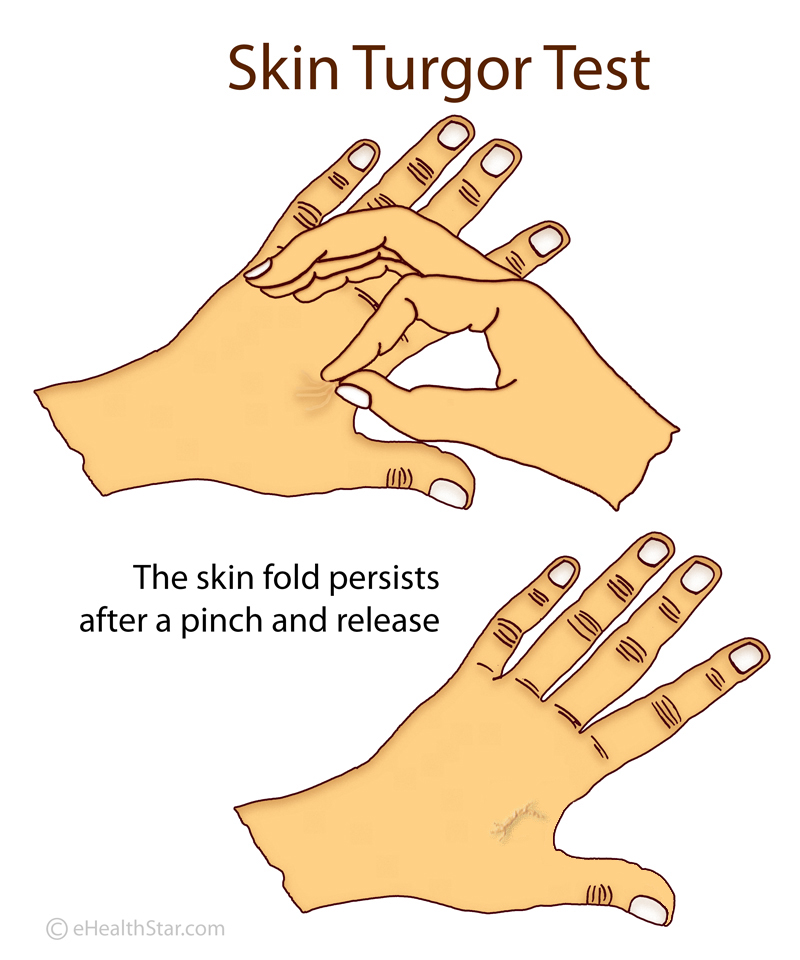 In healthy individuals, after a deformation or pinching, the skin quickly returns to its original shape. In patients with ALS, this return is slower. This is called the delayed return phenomenon (DRP).
In healthy individuals, after a deformation or pinching, the skin quickly returns to its original shape. In patients with ALS, this return is slower. This is called the delayed return phenomenon (DRP).
In the context of ALS, DRP has been associated with abnormalities in the dermal connective tissue, such as altered collagen composition. Microscopic examination reveals fewer and less organized collagen bundles and increasing gaps in the connective tissue. Electron microscopy shows the progressive deposition of fine materials in the dermal matrix, disrupting collagen fibers and connective tissue integrity. These changes reduce the skin's resilience and elasticity, making it softer and slower to regenerate.
ALS patients also exhibit decreased sweat gland nerve fiber density (SGND) and pilomotor nerve fiber density (PNF).
Histological studies show thickening of the walls of small dermal blood vessels, particularly in sporadic ALS (sALS). Electron microscopy reveals onion-like structures formed by β-amyloid deposits and basement membrane duplications, reducing the surface area of the vascular bed. This vascular remodeling, particularly in the papillary layer, may be linked to changes in autonomic innervation and contribute to preventing pressure ulcers.
One of the culprits for this state of affairs could be MMP-9, which belongs to the matrix metalloproteinase (MMP) family. Metalloproteinases degrade extracellular matrix components such as collagen. Proteins of the matrix metalloproteinase (MMP) family are involved in the restructuring of the extracellular matrix in processes such as embryonic development, wound healing, learning, and memory, as well as in pathological processes such as asthma, arthritis, intracerebral hemorrhage, and metastases.
